Over the last few years, medications like Ozempic® and Wegovy® have shifted how clinicians think about obesity and Type 2 diabetes. They belong to a class called GLP-1 receptor agonists – medicines that act on the same pathways as a gut hormone known as glucagon-like peptide-1.
For many people living with excess weight, repeated diets and exercise plans have not led to durable results. GLP-1 medications do not replace healthy habits, but they can make those changes feel more realistic and sustainable by calming “food noise,” stabilising blood sugar and improving how full the stomach feels after meals.
This guide walks through how GLP-1 medications work, how they interact with hunger hormones in the body, what kinds of results have been seen in research, and what to expect if you start one through a Vitercure care plan.
1. What are GLP-1 medications?
GLP-1 is a hormone naturally released from the gut after you eat. It helps:
- Signal to the brain that food has arrived.
- Tell the stomach to slow down how quickly it empties.
- Help the pancreas release insulin in a more controlled way when blood sugar rises.
GLP-1 medications are prescription drugs that mimic or enhance this hormone. They “plug in” to GLP-1 receptors around the body and are often given as injections once daily or once weekly. Some newer versions are being developed as oral tablets.
Common GLP-1 and GLP-1–like medicines include:
- Ozempic® (semaglutide) – approved for Type 2 diabetes, often used off-label for weight-loss in some regions.
- Wegovy® (semaglutide) – specifically approved for chronic weight management.
- Saxenda® (liraglutide) – a once-daily GLP-1 injection for weight-loss.
- Mounjaro® and Zepbound® (tirzepatide) – “dual incretin” medications that activate GLP-1 and another hormone called GIP.
- Trulicity® (dulaglutide) – a weekly GLP-1 injection for Type 2 diabetes with cardiometabolic benefits.
Each product has its own dosing schedule, pen device and approved uses, but they all lean on the same basic idea: support the body’s natural incretin system so that food, blood sugar and appetite are easier to handle.
2. Hunger hormones 101: how GLP-1 fits into the bigger picture
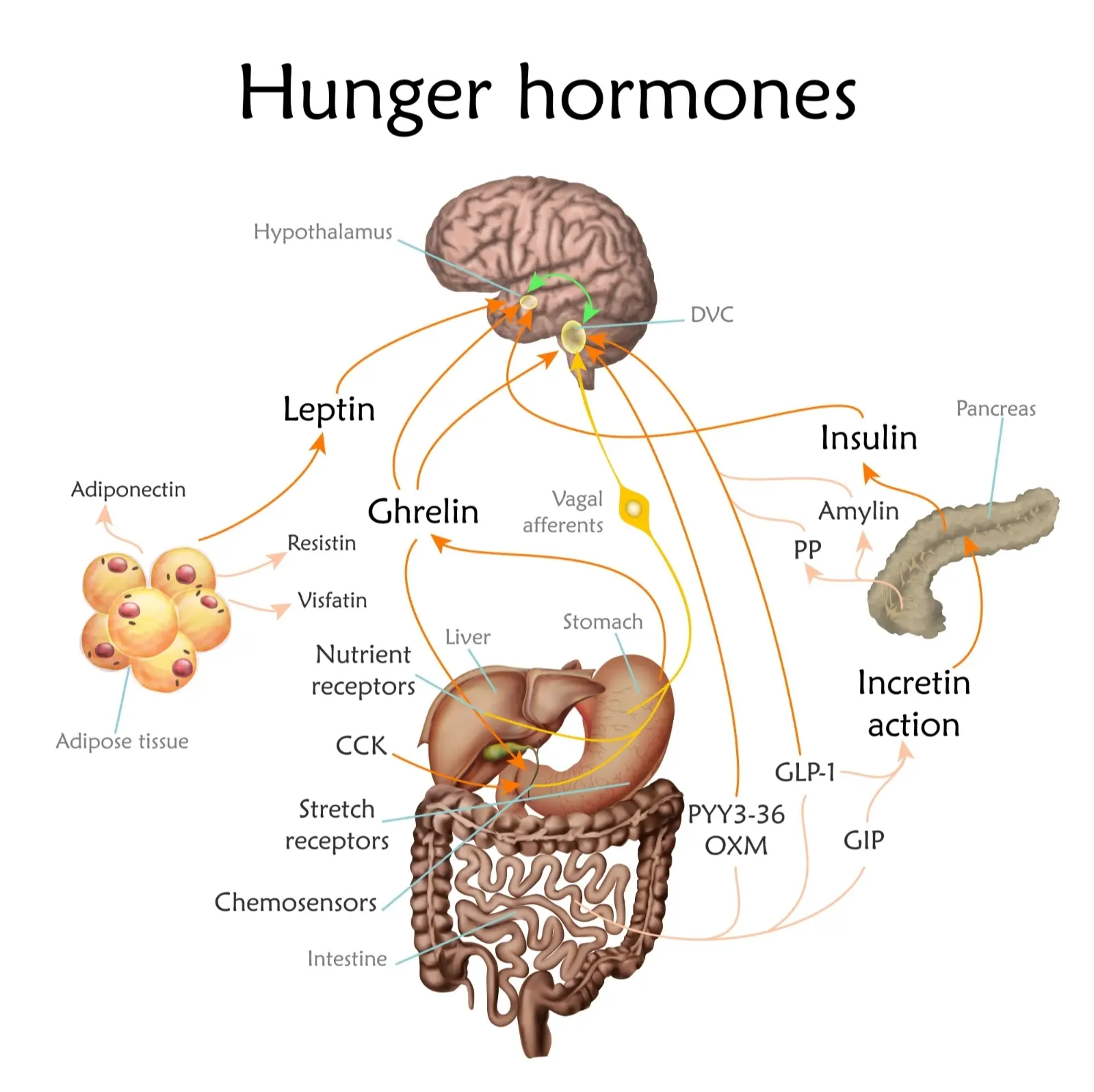
Your experience of being hungry or full is not just about willpower – it is heavily influenced by a network of hormones and brain signals. The image at the top of this article is one way to visualise how these signals move between the gut, pancreas, fat tissue and the brain.
Key players in hunger and fullness
- Ghrelin – often called the “hunger hormone.” Ghrelin spikes before meals and falls after you eat, nudging you to start looking for food.
- Leptin – produced by fat cells. In a healthy system, more stored fat leads to more leptin, which tells the brain to ease appetite. In obesity, the brain may become less sensitive to leptin (“leptin resistance”).
- Insulin – released by the pancreas when blood sugar rises. High insulin over long periods can be a sign of insulin resistance and is linked to weight gain and Type 2 diabetes.
- GLP-1 – released from the gut after food, acts on the pancreas, brain and stomach to moderate blood sugar and help you feel satisfied.
- Other incretins and gut hormones – such as GIP, PYY and CCK, which also influence fullness and digestion speed.
In many people living with obesity or long-standing insulin resistance, these systems are not sending clear signals. Hunger may remain high even when the body has plenty of stored energy. Fullness may fade quickly. Blood sugar may swing up and down, which can drive cravings for fast-acting carbohydrates.
GLP-1 medications do not “upgrade your willpower.” Instead, they help restore a more favourable hormonal environment so that the brain receives clearer messages about when you have eaten enough.
3. How GLP-1 medications support weight-loss
People often notice that, on an effective GLP-1 dose, they feel full sooner, stay full longer and experience less intrusive “food noise” in the background of their day. Under the surface, several mechanisms are working together.
1. Slower stomach emptying
GLP-1 receptor agonists signal the stomach to empty more slowly. Food spends more time in the upper part of the digestive tract rather than rushing quickly into the small intestine. This:
- Prevents sharp spikes in blood sugar after meals.
- Helps you feel pleasantly full after smaller portions.
- Reduces “crash hunger” that can occur when blood sugar peaks and then dips.
This is also why clinicians recommend eating smaller, slower meals on these medications. Very large, fast meals can increase the risk of nausea or reflux in some people.
2. Quieter hunger signals
GLP-1 receptors in parts of the brain related to appetite and reward help the brain listen to signals from the gut. When those receptors are activated by a GLP-1 medication:
- Baseline hunger tends to decrease.
- Cravings may feel less urgent or easier to delay.
- Some individuals report less emotional or “mindless” snacking.
This does not mean food loses all pleasure. It simply becomes easier to stop at enough, rather than constantly battling the feeling that you should keep eating.
3. Better blood sugar control
In Type 2 diabetes, the pancreas can struggle to release insulin in a timely, appropriate way. GLP-1 medications help:
- Increase insulin release when blood sugar is elevated.
- Reduce excess release of another hormone called glucagon, which otherwise raises blood sugar further.
- Improve overall insulin sensitivity over time in many patients.
When blood sugar is more stable, people often feel fewer crashes and less drive to reach for sugary snacks or drinks for quick energy.
4. What kind of weight-loss results have been seen in studies?
Individual results vary widely. No clinician can guarantee a specific amount of weight-loss for any one person. That said, large clinical trials give a sense of what is possible when GLP-1 medications are used along with nutrition and activity changes.
In several high-dose semaglutide studies for weight management, many participants lost a meaningful percentage of their starting body weight over many months. Some saw improvements in:
- Blood sugar and HbA1c (a marker of average blood glucose).
- Blood pressure and cholesterol levels.
- Markers of fatty liver and other cardiometabolic risks.
Dual-incretin medications like Mounjaro and Zepbound have also shown strong results in research, with some participants losing more weight than is typically seen with older medications alone.
5. Who may be a candidate for GLP-1 therapy?
GLP-1 medications are not appropriate for everyone, and different regions have specific regulatory criteria. Clinicians usually look at both body mass index (BMI) and weight-related health conditions when deciding who might benefit.
Common scenarios where clinicians may consider GLP-1 therapy
- Adults with Type 2 diabetes whose blood sugar is not adequately controlled with lifestyle changes and other medications.
- Adults with a BMI usually at or above a certain cut-off (often 27–30 kg/m² or higher) who also have weight-related conditions such as high blood pressure, high cholesterol or obstructive sleep apnoea.
- People who have tried structured lifestyle approaches and still find their appetite, cravings or metabolic markers very difficult to manage.
At Vitercure, your intake is reviewed by a licensed clinician before any medication is prescribed. They will look closely at:
- Your personal and family history (including thyroid and endocrine conditions).
- Past or current pancreatitis or gallbladder disease.
- Other medications you take that may interact with a GLP-1 medicine.
- Pregnancy, breastfeeding and plans for becoming pregnant.
- History of substance use or complex mental health concerns that require extra support.
Some people should avoid GLP-1 medications altogether, while others may be better matched to a different strategy such as metformin, SGLT2 inhibitors or, in selected cases, short-term appetite suppressants like phentermine.
6. What to expect when starting a GLP-1 medication with Vitercure
GLP-1 plans at Vitercure typically follow a step-up dosing schedule. You begin at a lower dose and increase gradually over several weeks or months. This gives the body time to adjust and can reduce the risk of stomach-related side effects.
Early changes many patients notice
- Feeling full after smaller meals.
- Less desire to graze between meals.
- Less intense cravings for highly processed or sugary foods.
- More even energy between meals if blood sugar becomes more stable.
Common short-term side effects can include:
- Mild nausea, especially after larger or richer meals.
- Changes in bowel habits (constipation or, less often, looser stools).
- Occasional burping or heartburn in some people.
- Decreased appetite that may feel surprisingly strong at first.
Your Vitercure care team will explain how to use the pen or device, how to rotate injection sites and how to store the medication safely. They may also suggest specific meal strategies – for example, focusing on protein, fibre and hydration, and avoiding very large, high-fat meals while your dose is increasing.
7. Why lifestyle changes still matter (even on a powerful medication)
It can be tempting to think of GLP-1 medications as a replacement for nutrition and movement. In reality, they work best as a tool that makes habit change more achievable, not as a stand-alone solution.
Four pillars Vitercure focuses on
1. Food quality and pattern
Because hunger is often calmer on GLP-1 therapy, this can be an ideal time to:
- Prioritise lean protein and plant-based proteins at most meals.
- Choose high-fibre carbohydrates such as vegetables, legumes and whole grains.
- Reduce ultra-processed snacks that give rapid spikes and crashes in both blood sugar and appetite.
- Eat slowly and stop when comfortably full, rather than aiming for a “stuffed” feeling.
2. Movement
GLP-1 medications can support weight-loss even without high levels of exercise, but movement remains critical for heart health, mood, bone strength and long-term weight maintenance. Your plan might include:
- Walking most days of the week.
- Simple resistance training at home or in a gym.
- Activities you genuinely enjoy, such as dancing, swimming or cycling.
3. Sleep and stress
Poor sleep and chronic stress can undermine any metabolic plan, with or without medication. Vitercure’s weight-loss education library explores sleep hygiene, stress-reduction techniques and ways to protect mental health while making big changes.
4. Long-term thinking
GLP-1 therapy is often most helpful when it is part of a multi-year strategy. Even if you do not stay on the medicine forever, the goal is to build skills and routines that continue after the prescription is adjusted or discontinued.
8. Choosing between Ozempic, Wegovy, Mounjaro, Zepbound and other options
There is no single “best” GLP-1 medication for everyone. The right choice depends on factors such as:
- Whether you are being treated primarily for Type 2 diabetes, weight-related health risks, or both.
- How often you prefer to inject (daily vs weekly).
- Insurance coverage, availability and pharmacy supply in your region.
- Your previous experience with any of these medications.
- Specific safety considerations reviewed by your clinician.
During a Vitercure consultation, your clinician may compare:
- Wegovy for chronic weight management.
- Ozempic when Type 2 diabetes and cardiovascular risk are major concerns.
- Mounjaro or Zepbound when dual-incretin therapy is appropriate.
- Saxenda or Trulicity if daily vs weekly dosing or particular insurance formularies matter.
In some cases, your provider may recommend starting with metformin or other foundational therapies first, then layering on a GLP-1 if needed. In other cases, a GLP-1 may be the preferred starting point because of your overall risk profile.
9. Quick GLP-1 FAQ
Does taking a GLP-1 mean I will be on it forever?
Not necessarily. Obesity and Type 2 diabetes are long-term conditions, and many people benefit from ongoing medication support, but that support may change over time. Some patients stay on a GLP-1 or dual-incretin medicine long-term; others gradually transition to different strategies as their health picture evolves.
Can I drink alcohol while taking a GLP-1 medication?
Moderate alcohol use is not automatically forbidden, but alcohol can interact with blood sugar, dehydration and stomach irritation – all of which are relevant on GLP-1 therapy. Many clinicians recommend drinking less or avoiding alcohol while starting or adjusting doses. Your Vitercure clinician will give you personalised guidance based on your history.
What happens if I miss a dose?
The answer depends on the specific medication and how much time has passed. Some weekly GLP-1s have clear instructions for what to do if you miss by a day or two. Others may require you to skip until the next scheduled dose. It is important not to “double up” on your own. If you are unsure, contact your Vitercure care team or your dispensing pharmacy for instructions.